Suboxone Treatment Withdrawal and Security System
In recent years, suboxone has become a popular go-to treatment for those struggling with opioid addiction. An addiction to opioids can develop for various reasons. For some, it arises out of treatment for chronic or acute pain. Prescription opioids are frequently used to treat chronic pain (from injury or an underlying medical condition) or as a short-term pain mitigation tool for someone recovering from surgery. Unfortunately, while these drugs are highly effective, they can also quickly become habit-forming and lead to dependence and addiction.
In addition to the overwhelming challenges presented by the opioid epidemic, millions also struggle with addictions to non-prescription opioids or “street drugs” such as heroin. Sometimes prescription medications like oxycontin are referred to as gateway drugs. They have gained this reputation because it is common for someone to turn to drugs like heroin after using prescription pain medication. The addictive qualities of heroin and other manufactured opioids are equally as potent as prescription drugs. Heroin is frequently used as a replacement once a prescription runs out or when the individual can no longer “get” prescription opioids. Suboxone is widely used in both residential and outpatient addiction treatment environments to help treat opioid dependence.
What is Suboxone Used for and How Does it Work?
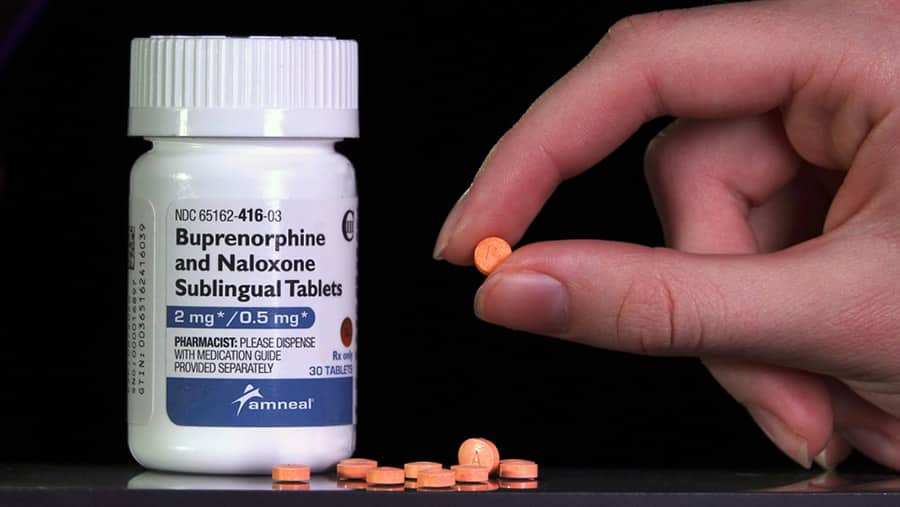
Suboxone is a combination of two medications, buprenorphine, and naloxone. Together, these drugs help chemically decrease the severity of withdrawal symptoms and reduce one’s dependence on opioids making the withdrawal process a bit easier. When you choose to seek help at an addiction treatment program where medically assisted detox is available, your treatment team may provide Suboxone medical guidance and supervision to reduce the intensity and severity of withdrawal symptoms. Reducing the discomfort often associated with opioid withdrawal can help make detox and withdrawal more manageable for most people.
Suboxone comes in two forms; a tablet and a dissolvable film that is placed in the mouth. Both forms are equally as effective, and the type each patient uses depends largely on the treatment center and personal preference. Suboxone works in the brain to reduce withdrawal symptoms and cravings in someone who is detoxing from opioids. The inner workings of how this medication interacts with the brain, however, is much more complex.
Within the brain, there are neurotransmitters. Neurotransmitters are known as the body’s “chemical messengers,” as they send signals and attach to various receptors throughout the brain. When an opioid is consumed, it reaches the neurotransmitters and is dispersed out to the opioid receptors. Activation of those receptors then occurs, signaling to the body that opioids are present, and symptoms develop such as euphoria, relaxation, and pain relief. When someone who is dependent on opioids suddenly stops abusing them, the opioid receptors get the signal that this type of drug is no longer being abused. This then promotes the development of withdrawal symptoms and cravings, which can be very painful and distracting.
Check Your Insurance Coverage for FREE
Find out if your insurance covers addiction treatment in minutes. We accept most insurance!
When Suboxone is being used as directed by a medical professional, the opioid receptors in the brain become partially activated without producing symptoms associated with “getting high” on opioids. Suboxone is known as a partial opioid agonist. This means the two components of Suboxone work together to block the receptors in the brain that function when opioids are present. This helps to decrease the pleasurable effects of opioids on the user. But what is a partial agonist? The best way to understand this is to think of the brain as the doorway to someone’s home. Without Suboxone working to limit access to the home, it is wide open for anything and anyone to enter.
Suboxone acts as a security system for the home. When someone recovering from opioid addiction takes Suboxone, it partially closes the door. Although some things may still enter, access is now limited and far more complicated. This action helps to calm withdrawal symptoms and cravings, making it easier for a person to detox and make their way into recovery. When someone takes Suboxone, it remains bound to the opioid receptors in the brain for several days. Therefore, if someone takes an opioid while Suboxone is still present in their system, it will block the effects of the opioid, making taking the drug less desirable and reducing use easier.
How Harmful is Suboxone Withdrawal?
Unfortunately, despite Suboxone being highly effective in treating symptoms related to opioid withdrawal, it is also a substance that can be abused. Suboxone is classified as a schedule III-controlled substance which means it is a drug with a moderate risk for addiction. Although suboxone is potentially addictive, the risk of addiction is generally less than other opioids. Buprenorphine, the opioid ingredient in suboxone, can cause moderate withdrawal symptoms should you suddenly stop taking suboxone2. Since Suboxone contains naloxone, however, it often takes a large amount of buprenorphine to create desired symptoms.
Unfortunately, those who are craving an opioid high and still struggling with an active opioid addiction will use higher amounts of Suboxone to get high. Continued abuse of Suboxone can quickly lead to addiction. Suboxone abuse includes taking more than prescribed or taking the medication in a way other than intended such as crushing and snorting pills or dissolving the strips and injecting them. Suboxone that is snorted or injected produces a much stronger high than results from taking the drug as prescribed, which can also lead to dependency and addiction.
The signs and symptoms of Suboxone addiction are similar to that of any other type of opioid addiction. The intensity and severity of withdrawal symptoms will vary based on a variety of factors, including the severity of addiction and individual characteristics of the individual. So, some people may experience far more severe symptoms than others. Physically, the person may appear to have dark, sunken eyes, poor hygiene, and a frail stature. They may struggle with fatigue, sleeping challenges, flu-like symptoms, digestive disturbances, and difficulties concentrating. From a psychological and emotional standpoint, the person may be anxious, depressed, have mood swings, and be detached from their surroundings. The most important thing that someone who is addicted to Suboxone can do is reach out for help, especially if they are dependent and are in need of detox services.
Anytime a person is dependent on a mind-altering substance, it means that their bodies and minds cannot properly function any longer without that substance. So, when someone who is dependent on Suboxone suddenly stops using, they develop withdrawal symptoms. These symptoms can become so distressing that a person might go right back to abusing Suboxone4 to get some relief. Unfortunately, this can increase their risk of overdose. Some of these symptoms can include, but are not limited to, the following:
- Stomach upset such as nausea, vomiting and diarrhea
- Headaches
- Sweats and chills
- Runny nose
- Watery eyes
- Abdominal pain
- New or worsening mental health conditions including depression and anxiety
- Difficulties sleeping
- Problems concentrating and other cognitive and memory challenges
- Intense cravings to use Suboxone (or other opioid drugs)
Suboxone withdrawal symptoms3 generally begin within twenty-four hours of one’s last dose. Like many other opioids drugs, they can occur sooner or take longer to present again, depending on the unique nature of the individual. The symptoms that a person develops tend to be reflective of the severity of their addiction. In other words, the more intense the Suboxone addiction, the more plentiful and painful these withdrawal symptoms can be. Typically, withdrawal symptoms last for seven to ten days, although they often decline in severity after the first three days. In some, less common cases, withdrawal symptoms can last for up to one month.
How Long Should You Take Suboxone?
Addiction and the process of overcoming addiction are different for everyone. As such, the duration of suboxone treatments will also vary. Depending on the severity of your addiction, suboxone treatments may last days, months or a year or more. In general, however, treatments typically last approximately one year. Studies indicate4 treatment outcomes are often better when suboxone interventions are maintained long-term. It is important to continue taking any addition treatment or mental health medication as prescribed by your provider.
Reach out to Hotel California by the Sea
We specialize in treating addiction and other co-occurring disorders, such as PTSD. Our Admissions specialists are available to walk you through the best options for treating your addiction.
When used as directed by your addiction treatment team, Suboxone can be highly beneficial as part of a comprehensive addiction treatment program. However, it is important to remember that its use is not without some risk. Although it does not produce the same high as opioid drugs, the effects of suboxone can lead to addiction if the drug is abused or misused. Someone who abuses suboxone regularly is at risk for becoming addicted. Some who are prescribed suboxone may take more of the drug than prescribed to achieve the opiate high they crave. Others abuse it by crushing and snorting the powder from prescribed pills or the film strips are dissolved and then injected. Suboxone that is snorted or injected produces a much stronger high than results from taking the drug as prescribed.
If you or a loved one are struggling with an addiction to opioids or suboxone, help is available to help you overcome your addiction and start over free from addiction. At an addiction treatment facility like Hotel California by the Sea, our caring and compassionate treatment team are here to help provide support and guidance as you begin your recovery journey. We provide comprehensive care beginning with medically supervised detox and continuing through all aspects of therapy and addiction education. Our admissions team and recovery professionals are here to make your recovery comfortable. Contact us at our Orange County, CA rehab today to learn more about how individualized treatment can help you overcome addiction.
References:
- https://www.nami.org/About-Mental-Illness/Treatments/Mental-Health-Medications/Types-of-Medication/Buprenorphine/Buprenorphine-Naloxone-(Suboxone)
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5855417/
- http://www.naabt.org/faq_answers.cfm?ID=70
- https://www.drugs.com/medical-answers/long-suboxone-start-working-3557484/